Related Links
Proliferative Diabetic Retinopathy
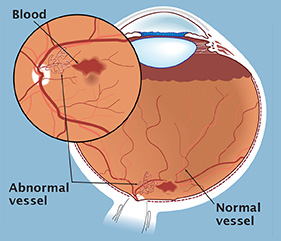
What is it?
When diabetes has been present for several years, problems with the retina (the membrane in the back of the eye which acts like camera film) can develop. While the exact cause of diabetic retinopathy is not known, it appears that elevated blood sugar levels can cause damage to the blood vessels and red blood cells, reducing circulation to the retina. These problems can probably be minimized by good long-term control of blood sugar.
In proliferative diabetic retinopathy abnormal blood vessels develop on the retina. These vessels can lead to visual loss through bleeding or scar tissue formation.
The new abnormal blood vessels on the retina do not improve circulation; in fact, they are fragile and can cause vitreous hemorrhage, or bleeding, which can reduce vision. Sometimes the blood vessels form scar tissue, which can pull on the retina causing retinal detachment.
Abnormal blood vessels in proliferative diabetic retinopathy can be detected in a routine exam by the ophthalmologist. Sometimes additional tests such as fluorescein angiography are used.
What causes the bleeding and how is it treated?
Bleeding in proliferative diabetic retinopathy comes from local factors in the eye including the abnormal blood vessels; it normally is not the result of unusual activity by the patient. The therapies for proliferative diabetic retinopathy include laser treatment, and injection of anti-VEGF (vascular endothelial growth factor) agents. If hemorrhage does occur, and does not clear, vitrectomy, or surgical removal of the blood can be done.
